Where to start… Life has been pretty complicated the last few months so I figure the best way to explain everything is with a list so hopefully it’s easier to understand. I’m also going to include add more links on my About My Conditions page with information about my newest diagnoses in case anyone wants to learn more.

Another Infection – For the last two weeks I’ve had a pretty painful chest cough and sinus issues. My doctor knew quickly that it was a bacterial sinus infection and bronchitis AGAIN and put me on antibiotics. I finished the first round of antibiotics but it still hasn’t cleared the infections. We’re trying a stronger, longer dose of oral antibiotics in the hopes that we can knock these infections out. It’s pretty common for me to get infections and also to need a second round of antibiotics to clear infections due to my immunodeficiency but hopefully this round is it because I don’t think my poor stomach could handle a third one.
Cardiology:
I’ve been receiving 1-2 liters of IV saline to help my POTS and minimize my fainting spells for the last two years through my central line. But in the last few months my fainting spells have changed and gotten worse. I have begun fainting even while laying down and sometimes I faint multiple times in a row. My heart rate has also been going between very drastic highs and lows, sometimes within the course of 5 minutes. I started seeing a new cardiologist and she is wonderful. Here’s a list of her current plan:
- Electrocardiogram – This was the first step and I had an abnormal EKG that showed premature ventricular contractions which led to further investigation.
- Echocardiogram – Results were inconclusive but pointed to possible issues with the function of my heart.
- 30 day cardiac monitor– What a long 30 days that was. Because of my corn allergy I am allergic to normal heart monitor electrodes and had to use pediatric sensitive skin electrodes. These do not stick very well and I had to replace them almost daily. I just finished wearing the monitor this weekend and received the preliminary results but we go Monday the 28th to discuss them with my cardiologist.
- New medication trial– I’m currently trying a combination of two medications to see if there is any improvement but in order to stay on them, my blood pressure has to stay above 100/60. I normally already have low blood pressure and so far during this trial my blood pressure has been too low. It has helped with my heart rate, taking it from its normal 90-100 bpm down to 50-60 bpm so I’m hoping we can find a way to make it work. It is great to not feel like my heart is racing 24/7.
- Stress test– This is the next BIG step but in early June I fainted and got a concussion by smacking the back of my head off of the ground. I have to receive a release from my neurologist and ENT before I am cleared to have a stress test.
- TEE (transesophageal echocardiogram) – After I’m able to complete and pass the stress test she wants to do a TEE because this will give her the ability to look at the structure and function of my heart.
Unfortunately right after starting with my new cardiologist I fainted and received my concussion. This isn’t the first time I’ve hit my head from fainting so I was stupid and stubborn and did not go to the ER until almost two weeks later. I knew I probably had a concussion but I did not take it that seriously because I had always heard they just need to heal on their own. Waiting that two weeks along with my complicated medical state already has made recovery much harder. So if you hit your head, PLEASE go see a doctor immediately! Now we are dealing with a mild traumatic brain injury (TBI) and all the new symptoms that come with it. Many of my current treatment plans need to be postponed until my head is able to heal and I am mostly symptom free.
ENT/Neurology:
At this point these are both really working together. I have had a lot of issues from my mild TBI but the most difficult ones for me have been the vertigo, nystagmus and sensory overload.
- Vertigo – We have been treating my vertigo with a medication called Meclizine since it was given to me by the ER doctor and it worked decently well. But when we met with the ENT we learned Meclizine has its downfalls. Meclizine works by blocking the signals to a patient’s brain so they don’t experience all of the symptoms of a TBI. BUT because the medicine only hides the symptoms instead of healing them, it is possible Meclizine is delaying my recovery and not actually helping me at all. The ENT does not believe I am stable enough to be taken off of Meclizine. Once I am it will still be a slow process because he fears my body will be overwhelmed by the symptoms all coming back at once. The hope is that when I finally stop taking Meclizine I will be able to start balance testing and also start vestibular rehab.
- Neuro MRI of brain, brain stem, and neck – This will check to make sure that there isn’t anything neurologically going on making the symptoms worse. It included a contrast study as well. Because I caught an infection, the MRI had been postponed several times but I was finally able to have it completed Tuesday night and we will have the results by next week. If my neurology MRI and 30 day cardiac monitor come back okay then I will be cleared to slowly stop Meclizine. Once I am off of Meclizine I will be able to do the balance testing then get clearance to do my cardiac stress test.
- Nystagmus – This is the biggest reason I have struggled so much to keep in contact with everyone. My eyes jerk quickly back and forth making it hard for me to focus and making my vertigo and headaches worse. The hope is this will resolve as my brain heals but I am seeing an optometrist who specializes in post-trauma vision syndrome on Sept 12.
Gastroenterology Motility:
For the last few years we’ve done a decent enough job maintaining my nutrition and weight. However, a never-ending gastroparesis flare that has lasted the entire summer has made maintaining my nutrition and weight impossible. In June I went back to Johns Hopkins to meet with my motility specialist and I received several new diagnoses but also a good plan going forward.
- Superior Mesenteric Artery Syndrome (SMAS): This rare condition occurs when the duodenum (the first part of the small intestine) is compressed between two arteries (the superior mesenteric artery and the aorta). This “pinch” causes a partial or complete blockage to the duodenum, further slowing down my digestion which is already very delayed due to my gastroparesis. SMAS happens due to the loss of the mesenteric fat pad which is the fatty tissue that surrounds the superior mesenteric artery. The minimum healthy SMA angle is 25 degrees. My last scan showed my SMA angle was only 15 degrees. This rare condition is most common in those who are petite like me and who have lost a good deal of weight in a short period of time. For the last two months I have been on a high protein diet (when my stomach could handle it) and a new medication to hopefully increase my appetite so I gain back that fat pad and increase my SMA angle. I recently had another Upper GI and small bowel series at Hopkins to check the angle again. The test results were inconclusive as small patients’ intestines are often compressed too tightly to be observed properly during the test. I have a follow-up with my doctor again in November to decide if I need to try a different type of testing, undergo surgery to place a feeding tube, or wait and try to gain more weight. In the meantime if I start to lose more weight or start having more issues eating, we are to email or call my motility specialist to talk about our options. But I cannot have any surgery without clearance from my cardiologist, ENT, and Neurologist which I will not be able to get until I complete all of their testing.
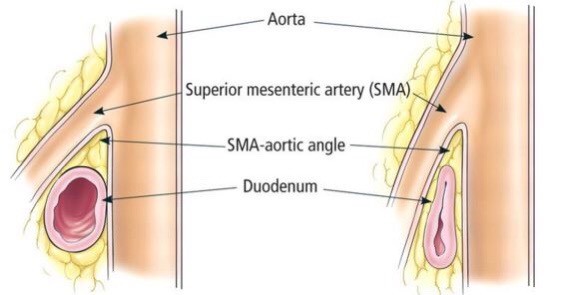
Illustration of Superior Mesenteric Artery Syndrome - EoE & EGID – Eosinophilic Esophagitis and Eosinophilic Gastrointestinal Disorders: These are new diagnoses that fall under gastrointestinal and immunology/allergy. EGIDs occur when a type of white blood cells called eosinophils builds up in the gastrointestinal system causing irritation and scarring of the esophagus and in some cases other parts of the digestive tract. EoE is the result of an allergy to a substance and the most common type of EGID. It can cause issues with swallowing, heartburn, and food getting stuck in the throat due to the inflammation. I’ve had issues with those symptoms for a while but somehow I was never told that my biopsy during my last scope was positive for Eosinophils in my esophagus, stomach, and small intestine. Ironically I have already been taking the recommended medications to treat these disorders because I take them for my Mast Cell Activation Syndrome but the best treatment is finding out what I am allergic to and avoiding it at all costs. My motility specialist wants to start working with my immunologist to see if they can come up with a good plan for management of EoE going forward and what approach to take to find out what new allergies I have developed that trigger it. At this point my known food allergies are corn, garlic, and onions (especially in the air) but clearly there are more since the EoE is not under control. With my current nutritional status, trying an elimination diet would be very hard but we are not new to food allergies, intolerance, or restrictions so I’m confident the right plan will fall into place and we will be able to handle whatever it may be.
My motility specialist at Hopkins has referred me to two clinical trials that she believes I am a good fit for. One is through Cleveland for the EoE which I would be able to do locally and the other is at Vanderbilt. Both have their benefits and risks but once we are able to get things semi under control, we may look into them further.
Allergy/Immunology:
- Idiopathic Angioedema: After having several angioedema attacks where my lips, throat, and tongue swelled and went numb, we were not able to find a common trigger for any of them. My immunologist believes they are not a new allergy or related to my Mast Cell Activation Syndrome. He believes that they are being caused by my immune system being over-reactive (which is slightly funny to me since I have an immunodeficiency. My immune system can’t fight bacteria but it can just freak out and go into an angioedema attack for no reason.) After a large increase in my daily antihistamines and adding even more pre and post IVIG IV steroids and IV Benadryl, these attacks seemed to be under control until about three weeks ago. I received IVIG and for the next 10 days went into angioedema attacks at least once a day, sometimes more. Each attack requires immediate IV Benadryl to get it until control and sometimes an ER visit for extra medications. When these attacks started in the spring, my immunologist was hoping they were temporary so he wanted to give it some time to see if they responded to the increase in medications. Since that doesn’t seem to be the case, we are going back for an appointment in a few weeks to discuss starting a new monthly immunotherapy shot called Xolair.
- IVIG– IVIG is still a roller coaster. I am doing biweekly infusions with half my monthly dose. For most of the summer, IVIG was going very well and although it was annoying to have to do them so often, I was finally having fewer side effects. Instead of feeling awful for at least a week afterwards and going into my “IVIG coma” as we call it, I was only sleeping about 2-3 days and felt decent after that. But after my last two IVIG’s, I have felt very sick like the way I used to feel and the chronic aseptic meningitis and migraines were worse than usual. This could be because of my TBI so we will see how things go once I am healed and back to “normal”. We may switch to my full monthly dose of IVIG once a month for the fall but the insurance process normally takes a while to switch things around which could mean missing infusions and I’m not sure I want to do that during cold and flu season. But switching to at home IVIG has been a great change. I’m lucky to have a great infusion nurse who I enjoy spending time with and who makes the time seem like it passes by much more quickly. And being able to snuggle with Addie on my own couch the whole time is always a bonus.

IVIG snuggles
Even though things are complicated currently, I have a great team of doctors who are all very caring, thorough, and want to improve my quality of life. It’s frustrating waiting for my brain to heal enough that I’m able to try all of these new treatment plans but I’m also hopeful that with this team I’m heading towards better control of my conditions which could open up a world of possibilities. This summer has definitely taught me a lot about humility and I’ve had to accept help doing most things when I didn’t want to. I’ve had to be more open with my doctors and stop always trying to be the easy patient. I’ve had to simply accept that I am not ever going to be the easy patient. I can still be the pleasant patient but there’s nothing easy about living with rare disease and I’ve only been hurting myself and delaying my care by not bringing up all of my concerns. And probably the hardest (literally) and most painful lesson I had to learn was that you should ALWAYS go get checked out after any type of head injury because there’s no such thing as “just a concussion” and waiting will only cause more problems.

It’s been to long. I just wanted to say I’m sorry and i think it’s time we act like sisters again and ki has his aunt back. We miss you
LikeLike